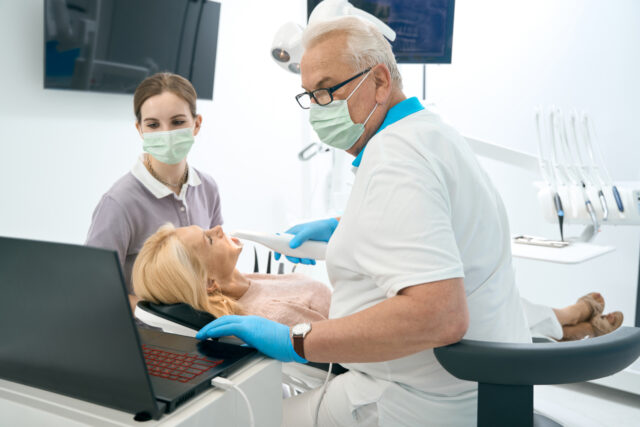
Even with advances in imaging, EHR systems, and clinical decision-making tools, diagnostic errors continue to quietly erode the credibility of care in dentistry. At Dentistry 411, we’re digging into new data that shows just how persistent — and preventable — these mistakes really are.
A recent analysis of over 58,000 paid dental malpractice claims shows that, while treatment-related claims dominate the malpractice landscape at 75.9%, diagnostic failures still account for nearly 9% of claims. These are real-world mistakes and common pitfalls that can lead to real patient harm, practice disruption, and long-term reputational and financial costs. Here’s what every dentist needs to know about these numbers, and what you can start doing differently right now to avoid becoming part of the next statistic.
Missed Diagnoses Are the Top Offender
Of all diagnostic-related claims, 78.6% stemmed from missed diagnoses. Delayed diagnoses followed at 13.4%, with outright misdiagnosis making up just 8%. That breakdown has remained remarkably stable over the decades, suggesting persistent vulnerabilities in early identification of disease or pathology.
This pattern aligns with broader medical literature where missed diagnoses consistently outnumber all other diagnostic errors. The implications are especially serious in dentistry, where delays in recognizing oral cancers, periapical pathologies, or progressive periodontitis can lead to irreversible outcomes for the patient.
What’s missing isn’t necessarily more information, but rather clinical attention to subtle or nonspecific signs, better documentation, and systems that prompt timely referral or follow-up. Diagnostic failures are often less about knowledge gaps and more about process failures.
The Demographics More Common in Claims
Demographics matter. The study found that most diagnostic claims involved:
- Female patients (59.7%)
- Patients aged 50–59 (22.2%)
- Providers aged 40–49 (29.4%)
- Dentists who graduated between 1970–1979 (27.4%)
- Providers practicing in the Northeastern U.S. (32.2%)
The overrepresentation of certain age groups on both sides suggests multiple contributors. Experienced dentists may face complacency or outdated diagnostic habits, while older patients may present with more complex cases that mask early signs.
Notably, male patients were statistically less likely to file diagnostic claims (IRR = 0.66), but that may be more reflective of utilization patterns than actual clinical outcomes. Female patients typically engage in more routine dental visits, creating more opportunities for both diagnosis and dissatisfaction.
Why Diagnostic Errors Still Slip Through the Cracks
The most likely culprits aren’t surprising: cognitive errors, system failures, and no-fault complexities.
- Cognitive bias remains a powerful driver. Anchoring on the most obvious diagnosis or failing to generate an adequate differential is a common clinical trap.
- System failures, such as missed follow-ups, poor inter-provider communication, or outdated technology, can derail even the best clinical instincts.
- No-fault errors, i.e., unusual presentations or very early disease, are real, but they’re not the bulk of these cases.
Interestingly, 46% of diagnostic error cases in broader healthcare have been attributed to a combination of systemic and cognitive errors. Technical proficiency isn’t enough. You need system-level safeguards to catch what human eyes might miss.
What You Can Do To Avoid Claims
Diagnostic errors don’t just hurt patients. They erode trust, invite scrutiny, and burden already strained dental teams with costly legal fallout. In some cases, they lead to settlements even when the original harm wasn’t egregious, simply because proper documentation or follow-up was lacking.
Here are a few practical takeaways you can tackle right now to lower your risk:
- Audit your diagnostic workflow, especially around high-risk areas like oral lesions, root pathology, and TMJ disorders.
- Standardize documentation of patient symptoms, radiographic findings, and follow-up recommendations.
- Implement recall systems that flag patients who miss key evaluations or referrals.
- Invest in ongoing training focused specifically on diagnostic acumen, not just new technologies or procedural skills.
- Encourage second opinions or case reviews, particularly in ambiguous or borderline diagnostic cases.
The 9% You Can’t Afford to Ignore
While diagnostic claims don’t represent the majority of malpractice suits, their impact is disproportionate. They’re harder to defend, more likely to involve serious harm, and often rooted in systemic issues that can affect multiple patients, not just the one who files a claim.
Improving diagnostic accuracy isn’t just about legal protection, but directly impacts your clinical reputation and patient trust. You’re likely already doing a lot right, but when nearly 1 in 11 claims point to a missed or delayed diagnosis, there’s still room to bridge the gap.
The most important takeaway from this review: Invest in systems and training that ensure nothing critical slips through. Because in dentistry, as in medicine, what you miss can hurt far more than what you treat.
Dentistry 411 will continue to track the science, the products, and the legal landscape so you don’t have to. Subscribe to stay ahead of the curve, cut through the marketing, and make smarter decisions in your dental practice.
SOURCES: JADA
Disclaimer:
The content provided in this article is for informational and educational purposes only and is not intended as legal advice. Nothing in this article should be interpreted as creating an attorney-client relationship. Readers should consult with a qualified attorney or legal professional for advice specific to their individual circumstances or any legal matters related to malpractice, liability, or risk management.